Introduction
Interstitial lung fibrosis is a chronic, progressive, and irreversible lung disease characterized by interstitial inflammation and excessive collagen deposition. It is known as the "cancer that is not cancer" and not only causes coughing and progressive respiratory distress in patients, but can also lead to respiratory failure in severe cases, becoming a "hidden killer" that threatens human respiratory health. At present, the pathogenesis of interstitial pulmonary fibrosis is not fully understood, clinical treatment methods are limited, and there is a lack of specific drugs. Therefore, building a stable and reliable model of interstitial pulmonary fibrosis has become a key approach to solving this disease problem. Animal models, as a "bridge" connecting basic research and clinical applications, can accurately simulate the pathological process of human interstitial pulmonary fibrosis, eliminate complex clinical interference factors, and provide a pure and controllable research carrier for scientific research work, which is the core prerequisite for promoting the landing of research in this field.
Today, we will comprehensively analyze animal models of interstitial pulmonary fibrosis to assist in scientific research and clinical cognitive upgrading.
Interstitial pulmonary fibrosis is a heterogeneous diffuse pulmonary parenchymal disease, characterized by abnormal proliferation of fibrous tissue replacing normal tissue to form "scars" (commonly known as "loofah lungs" or "honeycomb lungs") after lung tissue damage, resulting in loss of alveolar capillary function and ultimately leading to respiratory failure. The main symptoms in the early stage are persistent dry cough and shortness of breath after activity, which are easily misdiagnosed; Late stage respiratory distress worsens, accompanied by complications such as hemoptysis and clubbing.
From a clinical perspective, the etiology of interstitial pulmonary fibrosis is complex and diverse. Drug induction, environmental exposure, autoimmune diseases, genetic factors, etc. can all induce this disease. Among them, drug-induced lung injury (such as amiodarone, bleomycin, macromolecular antibody drugs, etc.) is one of the common clinical triggers, which poses great challenges to the safety of clinical medication.
The core of treating interstitial pulmonary fibrosis is to delay progression and improve quality of life, which is currently divided into four categories:
Traditional basic treatment
Mainly focused on oxygen inhalation, cough suppression, and avoidance of triggers, traditional hormones and immunosuppressants have been reduced in their individual use;
Targeted therapy
Nidanib and pirfenidone are core drugs that can slow down fibrosis progression and are clinically preferred;
New therapies
Stem cell therapy, novel small molecule drug therapy, and small nucleic acid drug therapy have become research hotspots, bringing new hope;
Integrated Traditional Chinese and Western Medicine Treatment
Synergistic efficiency and reduction of side effects
Lung transplantation is the ultimate choice for end-stage patients, but early diagnosis and intervention are still crucial due to limitations such as the donor.
Application scenarios of interstitial pulmonary fibrosis model
The interstitial pulmonary fibrosis model has a wide range of application scenarios in the scientific research field and has become a core tool for research in pharmacology, toxicology, respiratory diseases, and other related fields.
- Used to explore the pathogenesis of interstitial pulmonary fibrosis, including the regulatory mechanisms of core pathological processes such as inflammatory response, collagen deposition, and cell apoptosis;
- Screening and evaluation of new anti fibrotic drugs: By detecting the lung function, pathological morphology, molecular indicators, etc. of model animals, the therapeutic effect and safety of drugs are evaluated, providing reliable experimental basis for clinical drug development;
- Used for clinical drug safety research: simulating the process of damage to lung interstitium caused by drugs, environmental factors, etc., providing reference for rational drug use and environmental protection in clinical practice;
- Screening of diagnostic biomarkers for interstitial lung disease: assisting in early clinical diagnosis and disease monitoring, providing support for improving patient prognosis.
Case Study of Amiodarone Induced Interstitial Pulmonary Fibrosis Model in Rats
Data display
Changes in lung weight and analysis of inflammatory cells in bronchoalveolar lavage fluid
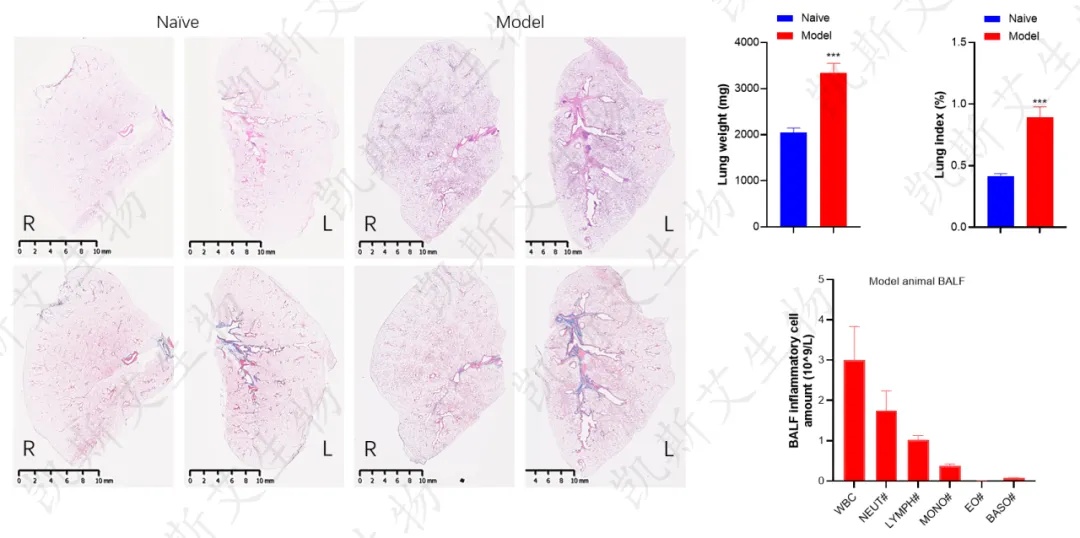
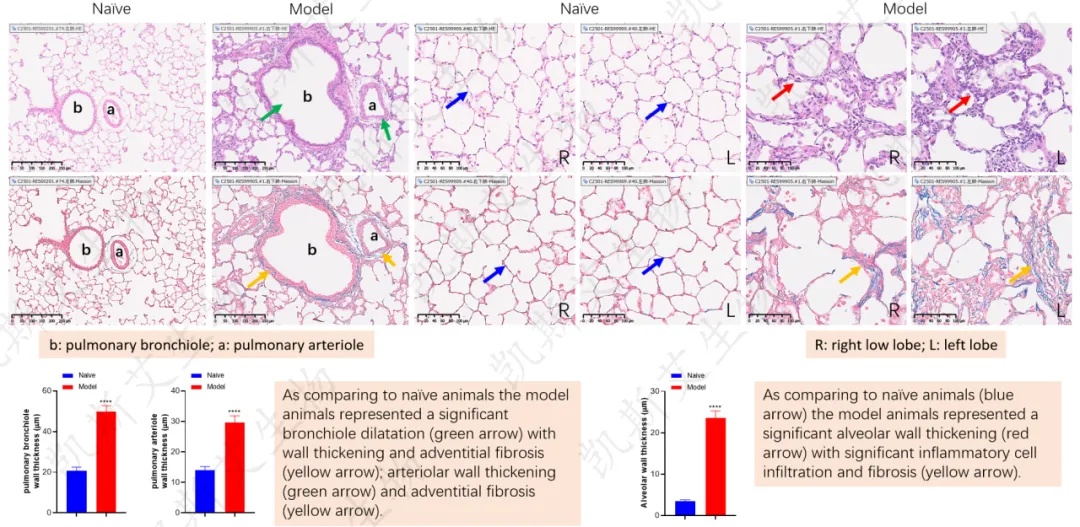
Pathological changes in the lungs
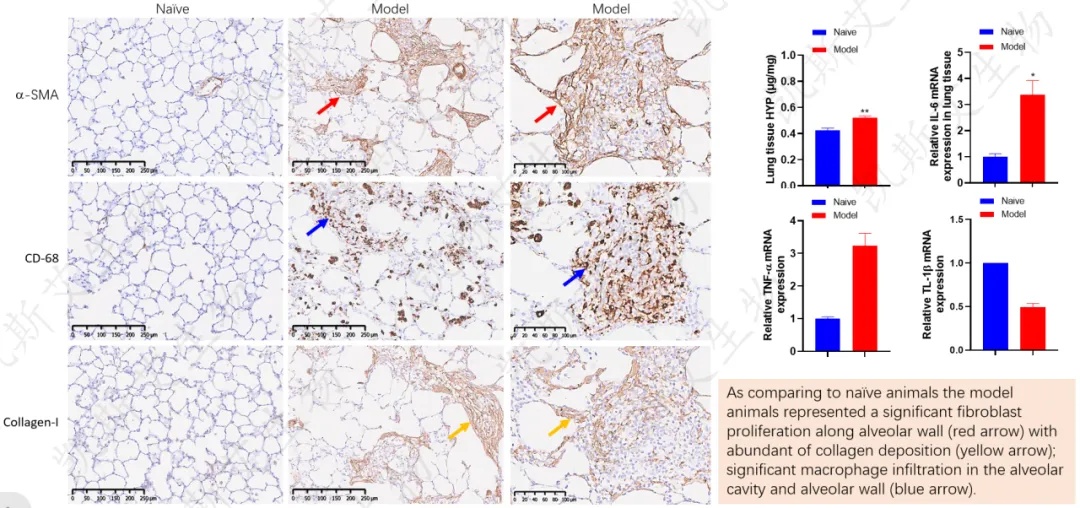
KCI•KMQ Respiratory Disease Pharmacodynamic Evaluation Platform
The KCI•KMQ Respiratory Disease Pharmacology and Pharmacology Evaluation Platform has a comprehensive animal model system and has accumulated rich project experience to meet diverse research needs. At present, the company has established extensive long-term cooperation with many well-known pharmaceutical companies and research institutions at home and abroad, providing a solid foundation for the development of innovative drugs.
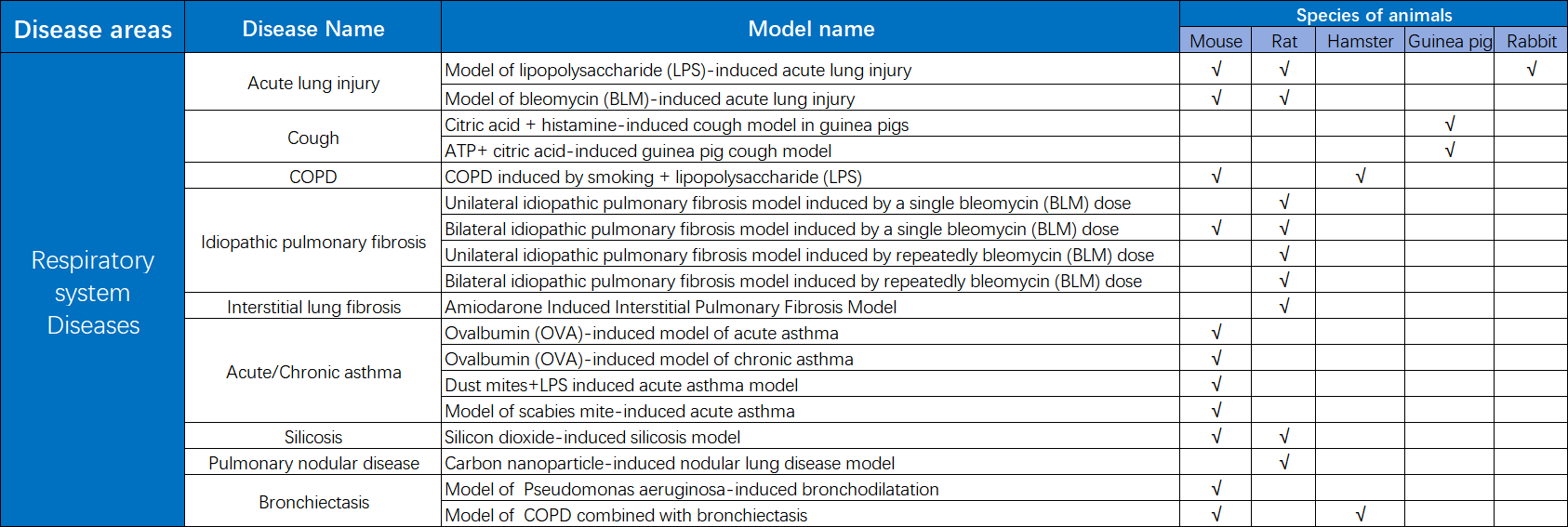
Summary
The value of animal models: a key bridge from mechanism analysis to clinical translation
The successful construction of an interstitial pulmonary fibrosis model is a key link between basic research and clinical application. Its stable and reliable characteristics can provide strong support for the study of the pathogenesis of interstitial pulmonary fibrosis, the development of anti fibrotic drugs, and the evaluation of clinical drug safety. KCI•KMQ animal disease models play a key role in this field, and with its professional model construction and evaluation system, it is continuously providing strong support for research institutions and pharmaceutical companies, jointly promoting the rapid transformation of respiratory disease from basic cognition to treatment breakthroughs.
If you need to obtain a detailed experimental plan for the model, please feel free to leave a message in the comment section, and we will answer your questions as soon as possible




